In Vanuatu, Few COVID-19 Cases But UNICEF Isn’t Resting Easy
The island nation has remained relatively unscathed throughout the pandemic, but that presents new hurdles as vaccination efforts begin.
No country has been untouched by the pandemic – but Vanuatu came closer than most.
Though the Pacific island nation has faced some disruptions in essential services and borders remain closed, COVID-19 is more a theoretical concern than a practical one for most communities here, compared to countries that have been hit harder. Thanks in part to strong national response, Vanuatu has had just three recorded cases to date. All of them were detected in quarantine, with no community transmission.
However, as vaccination efforts are underway through the COVAX Facility, Vanuatu could potentially be seen as a victim of its own success. UNICEF, the Ministry of Health and local partners now have a unique challenge in convincing the population to get vaccinated against a disease that feels very distant at the moment. We recently caught up with Eric Durpaire, UNICEF Pacific's Chief of Vanuatu Field Office, to learn more about the team’s ongoing response and why community outreach will be essential to keeping the country safe in the future.
Last year, we had heard about initial steps that you and your colleagues were taking to prepare for the pandemic. What have the last 16 months since then looked like? Has COVID been disruptive to your work?
ERIC DURPAIRE: With the national COVID emergency preparedness and response plan, UNICEF’s role was mainly focusing on WASH and the handwashing part, on training people in the hospitals on infection prevention and control, and on risk communication and community engagement. And all of these things are quite related. We worked closely with people in communities and in just a few weeks, we had handwashing stations everywhere.

Community mobilizers conduct handwashing demonstrations – one of the most effective ways of preventing the spread of COVID-19 – in Vanuatu’s Tekabu Community. © UNICEF/UNI316543/Pacific
In late March 2020, things became more complicated. The government closed the border. The period after this closure was quite stressful, because we were wondering if COVID was already here. The testing capacity was low. We had four weeks of sending tests to Australia, New Zealand or New Caledonia to see if it was here, even as the number of planes was much reduced.
On top of that, on April 6 Tropical Cyclone Harold devastated almost half of the country. Somehow, in that moment, we forgot the stresses of COVID, as we were responding to the consequences of Harold. It was a Category 5 tropical cyclone, a big one.
Tropical Cyclone Harold recovery efforts were made more complicated by the pandemic; emergency protocols made getting additional supplies into Vanuatu difficult
That must have been a lot to balance all at once. How did that impact the recovery?
DURPAIRE: Usually, in this situation, we receive surge assistance with a humanitarian team, WASH emergency specialists coming to assist, emergency supplies like tents and jerry cans — all things that are very useful for the response. But because the border was closed, we were not able to receive any assistance physically, and importing emergency supplies was challenging because of sanitary protocols put in place. In the beginning, people didn't know what treatment would be needed, so supplies would need to be disinfected before they were flown in, and people receiving them at the airport needed lots of personal protection. That was the situation.
Luckily, we also had a good pre-positioned stock of emergency supplies, so very quickly, with our small but committed team, we were still able to get support to communities.
With all of this uncertainty and upheaval, how were families feeling at the time? How was daily life disrupted?
DURPAIRE: They were very scared about COVID initially. Historically, Pacific islands during the height of colonialism had been highly affected by contagious disease brought by outsiders. You have this type of fear within the population, this historical memory that may not be tangible but is still deeply felt.
That said, Vanuatu has succeeded in staying relatively COVID-free. Geography has been a big factor; being an island is quite helpful. We also had good luck. COVID could have come with tourists early on. Thankfully that didn’t happen. People also had a chance to see that the quarantine system works very well. We only had three cases in this last year, and with the first case, there was a bit of a panic. Some schools closed, and everyone was worried. But soon it was clear that the detection system was working.
We are still COVID-free. That's very good news, and we are very happy about it. But the border is still closed, which is a concern now from an economic perspective because tourism is a significant part of people’s income in Vanuatu.
Vaccines arrived through COVAX in May, offering long-term protection and hope even as some remain skeptical
Now that vaccines are starting to arrive through COVAX, what does that mean for the population? How have vaccination efforts been going so far?
DURPAIRE: UNICEF is deeply involved in the vaccination plan and rollout plan here, and particularly within COVAX. We started to work last fall on a national vaccination deployment plan, and then we finally received the 24,000 first doses of AstraZeneca in mid-May. Vaccinations started on June 2.
Now the question is whether the entire population is willing to be vaccinated or not. As of July 3, about 12,000 people were vaccinated, which is a very good rate. We’ve focused on the frontliners – Ministry of Health staff, customs people, people working in the airport, in the seaport, in the quarantine, all these types. They are the ones to be vaccinated first, because without them, the system will collapse if COVID ever came here. And then the next group would be older and at-risk populations.
How are you adjusting the messaging compared to outreach efforts in countries that were hit much harder?
DURPAIRE: If you are skeptical about the COVID-19 vaccine, you’re asking yourself: What are the benefits to being vaccinated, and what are the risks? Obviously, the risks are very, very low, but because they are not under the direct threat of being sick with COVID, many may feel the benefit doesn't exist either. That's where our work in risk communication and community engagement comes in, to help explain that you do it for tomorrow, you do it for the future.
For instance, before vaccinations began, we had many briefing sessions with the Vanuatu Christian Council, who are the religious leaders of the country, and the National Council of Chiefs. We explained what we did know, but it was also very important to acknowledge that there are things we don't know. This situation is new. We don't know how long the efficiency of the vaccine will last. It's just the beginning.
On top of winning hearts and minds, you also have to contend with getting the vaccine to communities throughout Vanuatu. What does that involve when you’re working in a country made up of so many islands?
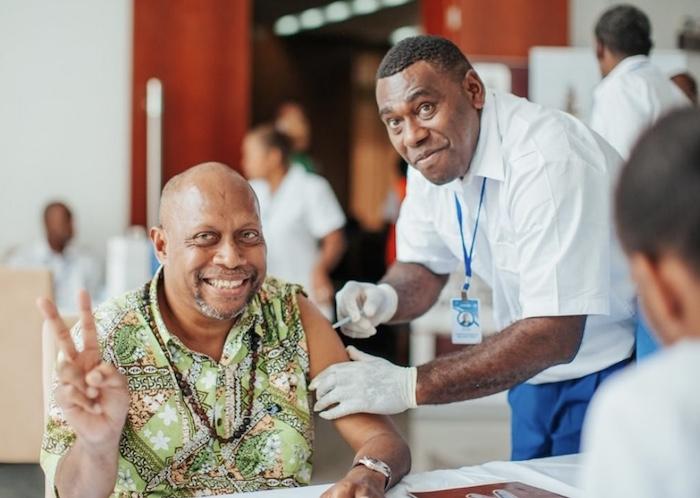
Senior government officials, community leaders and frontline workers, including health workers, were among the first to be vaccinated. © UNICEF Pacific/2021/Bax
DURPAIRE: For us here at UNICEF, the usual plan is really putting a strong emphasis on outreach to make sure that the last children in the last community will be reached. For instance, a couple years ago, we had drones in Vanuatu transporting vaccines in very remote areas.
But because of the nature of COVID, a remote village with 50 people is not at risk in the same way they would be with measles or polio. There is very little chance for COVID to go there, at least at the beginning. Instead, it is more important that those who need to be vaccinated will come to specific centers, and UNICEF is supporting the Ministry of Health to put in place buses to make sure that the people who are not able to travel on the own due to financial or health constraints could still come.
As vaccination efforts continue, more support is needed to make sure everyone throughout Vanuatu and around the world is protected. Take action now and urge your lawmakers to ensure equitable access to COVID-19 vaccines.
Top photo: "As frontline workers, it is paramount that we get vaccinated as we are most at risk of getting the virus. I am doing this to protect my family, my community and Vanuatu," says Joanne Mariasua, Acting Surveillance Manager at Vanuatu’s Ministry of Health (left). © UNICEF Pacific/2021/Bax
HOW TO HELP
There are many ways to make a difference
War, famine, poverty, natural disasters — threats to the world's children keep coming. But UNICEF won't stop working to keep children healthy and safe.
UNICEF works in over 190 countries and territories — more places than any other children's organization. UNICEF has the world's largest humanitarian warehouse and, when disaster strikes, can get supplies almost anywhere within 72 hours. Constantly innovating, always advocating for a better world for children, UNICEF works to ensure that every child can grow up healthy, educated, protected and respected.
Would you like to help give all children the opportunity to reach their full potential? There are many ways to get involved.