How Polio Paved the Way for a Powerful COVID-19 Response in Nigeria
An inside look at how UNICEF and partners in Nigeria’s successful fight to end polio were able to quickly pivot toward a new public health threat, applying many of the same tools and resources to addressing the COVID-19 pandemic.
UNICEF USA recently connected with Dr. Anisur Rahman Siddique and Muhamad Ridwan Hasan, key members of the UNICEF Nigeria team focused on polio eradication, for their insights into how the country has been able to leverage existing partnerships and platforms to strengthen its response to coronavirus. Here are excerpts from the conversation.
The global fight to end polio has been a massive undertaking — and a hugely successful one by many measures, in Nigeria and around the world. What tools and processes developed to fight polio are being leveraged today to tackle COVID-19?
DR. SIDDIQUE: All of them! In terms of leadership, in terms of process management, in terms of community support, all the structures for fighting polio in Nigeria have become the backbone for fighting COVID-19.

UNICEF-supported volunteers like Jummai, above left, have played a critical role in mobilizing communities behind polio immunization in Nigeria — and reaching otherwise hard-to-reach parents and caregivers like Ya Aisha, right, who is living at a camp for displaced families in northeast Borno State. Jummai visits about six families every day to discuss the importance of vaccinations and other best practices for keeping children healthy. Over 90 percent of Nigeria's volunteer community mobilizers (VCMs) are women. © UNICEF/UN0353340/Herwig
We have a polio emergency operations center where all the partners can get together and work out a strategy for the mission in a cohesive manner. This is important. We have an operations group and a logistics committee. There’s a presidential task force for polio, and UNICEF and other partners in the Global Polio Eradication Initiative [GPEI] are part of it. When COVID struck in early March of 2020, that task force was immediately converted into a presidential task force for COVID. So from a policy perspective, and on the governance side, we were able to leverage that existing polio platform and all the learning that came with those past activities.
A task force pivots, leveraging existing resources
And all the subgroups that had been created — surveillance, epidemiology, infection prevention, risk communication and community engagement — all pivoted toward responding to COVID. The whole COVID task force was built right on top of that existing infrastructure.
I’d say 60 to 70 percent of our human resources have been diverted to the COVID response. We have about 20,000 UNICEF-trained volunteers on the ground, who are from the communities they work in, and they immediately got on board, propagating messages around COVID — the importance of social distancing, of handwashing with soap and so on.
UNICEF helped create a questionnaire to gauge public understanding and awareness of COVID-19, and our C4D [Communication for Development] team developed messaging and risk communication materials based on the responses. The World Health Organization has its own team of informants who work the surveillance side. These key informants immediately started contact tracing and reporting COVID cases.
Applying lessons already learned delivering vaccines and services to children in hard-to-reach places
We were also able to leverage all the learning that came from having to figure out how to deliver polio vaccines to children in hard-to-reach places, especially children living near and around the conflict in Borno, the state in the northeast where the Islamist insurgent group Boko Haram is active. And we are getting better on the service delivery side.
Wasn’t that the GPEI's original vision, to build up this infrastructure and establish these systems that can then be tapped and repurposed as needed?
MR. HASAN: Yes. It made perfect sense to tap into our polio resources and systems to respond to the COVID-19 outbreak. And it’s the not the first time we’ve leveraged them; they’ve helped us combat measles, for example, and strengthen routine immunizations.

Volunteer vaccinators in Nigeria carry polio vaccines in cold boxes like this one as they go door to door to immunize children. © UNICEF/UN0353362/Herwig
Our 20,000 volunteer community mobilizers, or VCMs for short, have always gone above and beyond the polio mission. They work in 12 states that are considered high risk for polio, states in the north, including Borno where there are highly insecure areas. As they go door to door in the communities, talking to caregivers and administering the oral polio vaccine, they also promote other health campaigns. They refer pregnant women for antenatal care services, which is critical for maternal health, for example. They promote routine immunization by referring caregivers to the local health facility to get their children vaccinated for other diseases like diphtheria and rotavirus. And they follow up when caregivers are noncompliant.
UNICEF's vast network of community volunteers proves invaluable
In 2020, our network of volunteers reached anywhere between 600,000 and 1.7 million caregivers in a given month, which translates into more than 1.65 million children getting vaccinated for polio — while increasing the likelihood that those same kids will receive additional health services because of the information given at the time of the home visit. VCMs also record their activities and the families they visit, and this data helps us gauge how a community is faring on several different health indicators.
And they didn't stop their community outreach when COVID hit.
MR. HASAN: No, they kept at it, shifting to a COVID-focused role.
And when the pandemic hit, many immunization and health care services not related to COVID were strained or interrupted, not only in Nigeria but in a lot of countries, isn't that right?
DR. SIDDIQUE: It’s true that when COVID came in March 2020, we paused all other campaigns, including two polio vaccination campaigns we had planned for that April and May. There was a lot of fear among caregivers and among service providers at that time, as you can imagine. There was fear around what to do, what was safe. There wasn’t enough PPE [Personal Protective Equipment] to go around at first.
Of course we were gravely concerned that all the gains we had achieved in immunizing children against polio would be reversed. But we have been able to catch up to a large extent since. I’d say that 75 percent or so of the children we missed last year have been vaccinated.

Umme, 4, from Fanisau Ugongo Village in Kano State, Nigeria, attends a community meeting about the importance of child immunizations, organized by local women and led by a UNICEF-trained volunteer community mobilizer. VCMs have built critical relationships with traditional leaders and other local influencers to build trust in the polio vaccine — relationships they have since leveraged to help raise awareness about COVID-19 prevention and strengthen the country's overall response to the pandemic. © UNICEF/UN0353360/Herwig
In some ways the interruption was a good thing, because it forced us to reevaluate our approach. It had become obvious that the polio-specific campaign approach was no longer going to work in the new country context, in a COVID context. So we have started to shift vaccine delivery to PHC [primary health care] workers — to make polio a routine vaccination, in addition to conducting outbreak response campaigns as required. House to house campaigns are how we make sure every child is getting the polio vaccine — which can be administered on the spot — but we also use the same house to house approach when there is an outbreak of measles or yellow fever, though the vaccines for those must be given at a facility.
Strategy for keeping Africa polio free: ensure routine immunization for all children
We call this integrated medical outreach and it’s an innovative approach, community based not campaign based. The whole idea is that the polio team will support PHC services and PHC will become the focal point for immunizations. The polio vaccine becomes part of a package of care services. This is how we keep Nigeria — and all of Africa — free from all forms of polio.
The key to making this work is engaging faith-based organizations, traditional leaders and local influencers. I’m not saying it’s foolproof. We have a lot of areas we still need to improve.
Do you encounter much vaccine hesitancy or mistrust of vaccines in Nigeria? How do you deal with that?
MR. HASAN: Vaccine hesitancy in Nigeria has always been a problem. Fortunately for polio, because of our close community engagement through the volunteer community mobilizers, and because of our strategic partnership with the northern traditional leaders, the trust in the oral polio vaccine is very high. It is the most familiar of all the vaccines to caregivers.
Trust in vaccines can vary depending on the antigen, how it is administered, etc. An oral vaccine is easier to administer than an injectable one, and that is more appealing to some people.
There have been some rumors and misinformation, especially around COVID-19 vaccines. We work closely with the National Primary Health Care Development Agency to debunk misperceptions and myths around COVID-19 vaccines through social media and other channels.
DR. SIDDIQUE: It can be a bit more difficult to get a read on hesitancy with the COVID vaccine. With polio, with our teams going house to house, you know when a family is refusing it. With COVID, you don’t really know how many people are actively choosing not to come to the facility to receive their COVID vaccine.
We received our first shipment from COVAX on March 2, and since then vaccinations have been picking up. But there is some uncertainty as to how quickly we will be receiving more doses. We don’t want to generate demand for the COVID-19 vaccine unless we have enough supply on hand to meet it. It’s a balancing act.
Learn more about UNICEF’s role in COVAX, supporting global equitable distribution of COVID-19 vaccines.
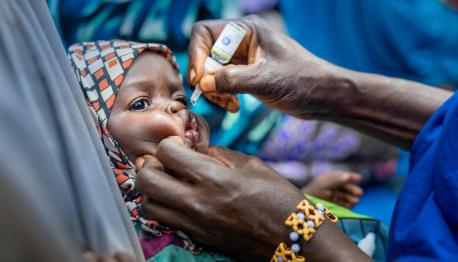
Top photo: A volunteer community mobilizer (VCM) administers the oral polio vaccine to a child in Fanisau Ugongo Village, Kano State, Nigeria. VCMs often take advantage of community gatherings such as naming ceremonies and other events to talk with parents and caregivers about vaccination and other healthy practices. © UNICEF/UN0353359/Herwig


