Maternal Health: What We Should Know
Healthy pregnancies lead to healthy mothers and a good start for newborns, but not all moms and babies receive the same level of care. A look at how the U.S. health care system is failing Black mothers and mothers-to-be, and how UNICEF is working to improve outcomes for mothers and babies around the world.
A year ago, I hosted a UNICEF Next Generation event where we discussed maternal health and the disparities Black women face in the U.S. health care system. Our goal was to raise awareness, educate our community and advocate for better maternal health policies. Little did I know that nine months later, I would end up in an emergency room for close to 10 hours in excruciating pain with complications from a procedure following a missed miscarriage — only to be discharged with barely any information besides instructions to follow up with my ob-gyn in a few days.
A missed miscarriage, sometimes referred to as a silent miscarriage, occurs when the embryo or fetus is no longer alive but the usual symptoms of a miscarriage such as cramping and bleeding do not occur. As soon as I learned that I had had a silent miscarriage, I scheduled a procedure to remove the embryo – which I had already begun to think of as my baby. Four days after the procedure, I woke up to severe cramping and immediately knew something was wrong.
I woke up to severe cramping and immediately knew something was wrong.
My husband and I decided to go to the emergency room five minutes from our apartment and called my doctor’s office to speak with the on-call ob-gyn for guidance. My doctor was not affiliated with the hospital and we knew how Black women like myself are often treated by the health care system, so we wanted to make sure she was aware of the situation and that I would receive the proper care. Luckily for me, my ob-gyn was the doctor on call that weekend.
An ultrasound at the hospital confirmed that I had either blood clots, remaining pregnancy tissue or both. We called my doctor to tell her the results, and she firmly stated that I should not be discharged without clear next steps on a solution to prevent the risk of infection.
After 10 hours in the ER and only one short conversation with the ER doctor, I was told that I was being discharged. When my husband and I asked the nurse why, because we were still unsure of what was happening, she replied, "I don't know." We asked for more information and were given a copy of my ultrasound results, a prescription for pain medication, and instructions to follow up with my doctor in a couple of days. I left the ER still in pain and still unsure if I had remaining pregnancy tissue and needed surgery right away to remove it, blood clots or both.
Upon arriving home, I immediately called my doctor. Shocked that I had been discharged with so little information, she advised me to immediately send her my ultrasound results. She told me I only had minimal pregnancy tissue left and some blood clots, and that a procedure was not needed. She provided me with medication so that my body was able to release everything. She reassured me that everything was going to be okay and checked in on me during the next 48 hours to ensure I did not have any additional complications.
Around the world, about 810 women die every day from preventable complications related to pregnancy or childbirth
What I experienced is what many women, especially Black women, experience in our health care system: lack of proper health care, implicit bias and more. Yet I still consider myself one of the lucky ones. Globally, approximately 810 women die each day from preventable complications related to pregnancy or childbirth. According to the Centers for Disease Control and Prevention (CDC), 658 women died of maternal causes in the U.S. in 2018. The maternal mortality rate for black women was more than double that of white women at 37.1 deaths per 100,000 live births compared to 14.7.
The novel coronavirus has created new concerns regarding the health of pregnant women and the care they receive. The reality is, very little has improved when it comes to the overall issue of maternal health. The COVID-19 pandemic has only exacerbated the existing challenges we face when it comes to maternal health. It has also highlighted what many of us always knew: We are failing our mothers and mothers-to-be.
When we look at maternal health, it’s important that we look at social determinants that impact health outcomes such as individual and cultural behaviors, economics and system barriers. How does the environment in which we live impact our health? Where systems were weak, they became weaker with COVID-19. Do we have enough health clinics, and if so, is access limited to those with health insurance? Are the health clinics located in remote areas that are difficult for women to reach? In the U.S., there are racial and financial barriers along with lack of access. In order to improve maternal health, we need to look at the issue through a holistic lens.

On October 23, 2019, nurse Hindia Al-Zoubah checks on a 5-day-old baby girl who is making good progress in the neonatal intensive care unit at UNICEF-supported Al Sabeen Maternal Hospital in Sana’a, Yemen. © UNICEF/UNI314576
According to the World Health Organization, the complications that account for nearly 75 percent of all maternal deaths are severe bleeding, mostly after childbirth; infections and high blood pressure during pregnancy leading to pre-eclampsia. We’ve heard stories about Serena Williams, Kira Johnson and most recently Amber Isaac. Isaac’s platelet levels had been dropping since February of this year, but because of the pandemic she had video meetings with her doctors instead of meeting with them in person. By the time doctors finally agreed to see Isaacs in person in April, it was too late. She passed away during childbirth. In the U.S., organizations like March of Dimes, Every Mother Counts, the Black Mamas Matter Alliance and 4Kira4Moms have been advocating for better maternal health policies, providing support and resources and educating our communities on the impacts of maternal mortality.
UNICEF works with partners to increase access to affordable and quality health care for mothers and newborns
UNICEF partners with governments to address the inequities in accessing affordable and quality health care to help improve maternal and newborn survival – working to ensure women receive quality prenatal and postnatal care. UNICEF also works to improve maternal nutrition, ensuring pregnant women have equitable access to good nutrition. In many countries, UNICEF works with local government to set up a network of community health workers who make home visits.
Weak health systems result in missed opportunities at the facility level, so UNICEF has identified the need to meet mothers and babies where they're at — in their communities. This is very important, particularly in rural communities where transit, financial resources and education barriers might otherwise keep mothers from getting the information they need to stay healthy and keep their newborns healthy.
Especially during these challenging times, it’s really important to make sure we support pregnant women, advocate for them and encourage them to advocate for themselves. Look to organizations, programs and health departments such as Nurse-Family Partnership, Office on Women’s Health and the U.S Department of Health & Human Services for helpful resources and guidance. Midwives and doulas have also been a major source of support for many pregnant moms.
Learn more on how to navigate pregnancy during the COVID-19 pandemic.
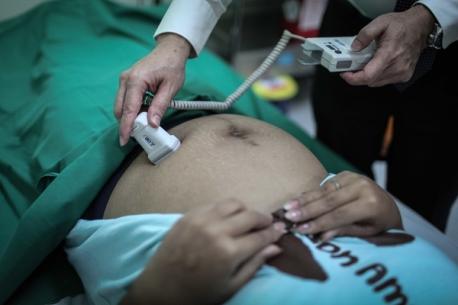
Top photo: A doctor examines an HIV-positive pregnant woman at Siriraj Hospital in Bangkok.© UNICEF/UN040402/Preechapanich


