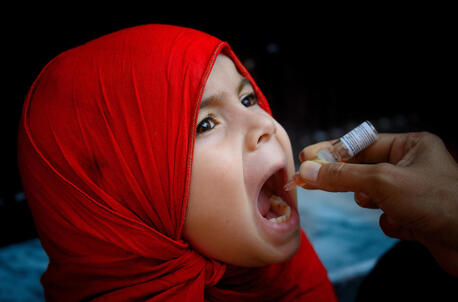
6 Ways the Fight Against Polio Is Transforming Global Health
Innovative methods and a disease-fighting infrastructure developed in the battle to eradicate polio are creating lasting impact in other areas of public health.
When the largest Ebola outbreak in history swept through West Africa in 2014, health workers used methods refined in the fight against polio to keep the virus from gaining a foothold in Nigeria: replicating a polio outbreak Emergency Operations Center, identifying and monitoring contacts of Ebola patients, and engaging in extensive public communication.
Social mobilization teams reached out to at-risk groups and key community leaders to dispel rumors and teach people how to prevent the spread of Ebola. The rapid response limited the outbreak in Nigeria to only 19 confirmed cases and halted widespread transmission. The successful containment was proof positive that lessons learned in the battle to eliminate polio are transforming global health care.
Polio may soon be a thing of the past, but the innovative methods and infrastructure developed to eradicate it will have a lasting impact. In addition to ensuring every child receives a polio vaccine, health workers are also working on other public health efforts. The polio network is being used to immunize children against other diseases, fight outbreaks and respond to natural disasters. New medical technology such as robot blood testers and needle-free devices utilized in the fight against polio will continue to be used to address other health issues.
1. Diversifying the polio network's mission
When the Global Polio Eradication Initiative (GPEI) was formed in 1988, poliomyelitis paralyzed more than 350,000 people a year in 125 countries. Since then, history's largest internationally coordinated public health effort has reduced the number of polio cases by an astonishing 99.9 percent.
Led by national governments with five core partners — The World Health Organization (WHO), Rotary International, the US Centers for Disease Control and Prevention (CDC), UNICEF and the Bill & Melinda Gates Foundation — GPEI, with the help of more than 20 million volunteers worldwide, has saved more than 16 million people from paralysis. Today, the virus is endemic in only three countries: Afghanistan, Pakistan and Nigeria. In 2016, only 37 cases were reported worldwide.
In the 21st century, diseases have the potential to spread farther and faster than ever before. Since March 2014, at least 140 serious outbreaks in 107 countries have received global attention: Ebola, Avian Flu, MERS, Zika. Polio workers are stepping in to share their expertise. In Ethiopia, polio staff have worked to control cholera outbreaks, and in Angola, health workers relied on communications infrastructure set up by polio teams to monitor and control an outbreak of Marburg fever.

A UNICEF-supported polio team goes door-to-door to vaccinate young children in the urban Peshawar, Pakistan. © UNICEF/UN0127379
2. Cross-country coordination
Two countries, one team. Afghanistan and Pakistan share a border — and a lingering polio problem. As migrant groups travel freely between the two countries, the virus moves with them. Since 2015, polio teams on both sides of the border have closely coordinated their immunization strategy to be certain that no child in the region is left unvaccinated. An integrated communications campaign uses weekly radio health shows and soap opera storylines emphasizing polio and children’s health to educate Afghans and Pakistanis on the importance of immunization. Methods developed to synchronize polio eradication services and messaging between countries will be invaluable in other public health initiatives around the world.
3. Strengthening surveillance and knowledge
International consultants are stationed around the world in the countries most vulnerable to polio. To coordinate their efforts, consultants use a cellphone data reporting application, Survey123. The app captures data in real-time to track the virus, record immunization coverage, identify immunity gaps and support vaccination campaigns to fill them. The polio lab and surveillance network currently includes over 140 labs and is linked to the global measles/rubella and yellow fever lab networks. Polio field workers have led the march in reporting and responding to other priority diseases. Nepal’s polio eradication program, for example, has been reporting on cases of measles, rubella, neonatal tetanus and Japanese encephalitis since 2004.

A volunteer uses chalk to record polio immunization data on a house wall in Tashan Damboa, Borno State, Nigeria. © UNICEF/UN036826/Abubakar
4. New uses for robotic technology
The CDC's Population Immunity Team uses automated laboratory machines to test blood samples for poliovirus antibodies through a process called serological testing. These robots have significantly expedited the number of samples processed — from 20,000 to 30,000 in two decades combined to 100,000 samples in 2012 alone. The machines not only accelerate the rate of sampling, they also produce more accurate test results. The robots have the potential to benefit other disease programs, including measles and Zika.
5. Adapting innovative delivery systems
New needle-free devices and micropatch needles are revolutionizing the way polio vaccines are administered. The PharmaJet Tropis needle-free device delivers vaccines intradermally through a narrow, high velocity stream of fluid that penetrates the skin without the use of a needle. While health workers will still need special training, the use of these devices could make their lives easier, and they can be used for other vaccines as well.
Micropatch needles are also being developed by the Georgia Institute of Technology and the CDC. Each patch, about a square inch in size, contains 100 solid, conical microneedles made of polymer, sugar and vaccine, each the diameter of a human hair. When pressed into the skin, the needles dissolve, leaving only the patch backing. Researchers are also studying microneedle administration of the measles, influenza, rotavirus and turberculosis vaccines.
6. Leveraging vaccination teams
In parts of the world where the health infrastructure is weak, polio vaccination teams deliver other much-needed health care services at very little additional cost. In remote villages, they screen children for malnutrition, administer routine immunizations and distribute vitamin A, which gives a general boost to immunity and helps children fend off a range of infections. To date, an estimated 1.5 million childhood deaths have been prevented through the systematic administration of vitamin A during polio immunization activities.
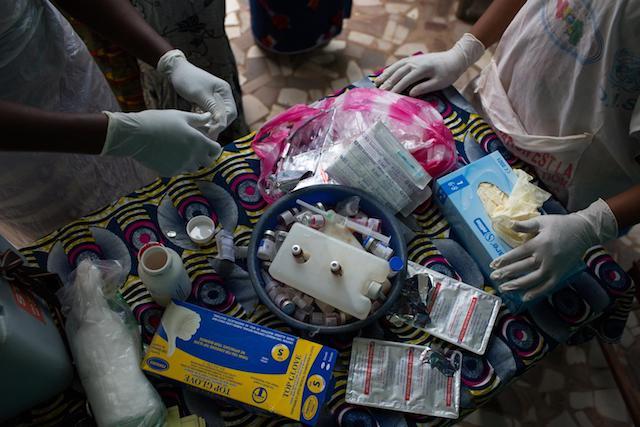
Nurses prepare to vaccinate children against polio and measles and administer deworming pills and Vitamin A at the Madina Health Center in Guéckédou, Guinea. © UNICEF/UNI183268/Bindra
Thanks to the innovative and carefully coordinated efforts of heath care workers worldwide, polio's eradication is at last in sight. The knowledge, resources and infrastructure developed to end polio will continue to prove invaluable in protecting children from other diseases and improving their lives for decades to come.
Learn more about UNICEF and Rotary International's efforts to eradicate polio.
Banner photo, top: Polio vaccinator Aisha Bulama, center, was part of a massive emergency immunization campaign supported by UNICEF and partners in 2016 that delivered polio vaccines to children under the age of 5 in high-risk areas in Nigeria, Chad, Niger, Cameroon and Central African Republic. Photographed on October 15, 2016 in Maiduguri Metropolitan Council, Borno State, Nigeria, Bulama said proudly, "My team has already vaccinated over 500 children in just a few hours." © UNICEF/UN035993/Page